 Alopecia areata (AA) is a chronic autoimmune disorder that causes non-scarring hair loss. It affects approximately 2% of the global population and can range from small, patchy bald areas to complete loss of scalp and body hair. The disease is unpredictable and may have a significant emotional and psychological impact.
Alopecia areata (AA) is a chronic autoimmune disorder that causes non-scarring hair loss. It affects approximately 2% of the global population and can range from small, patchy bald areas to complete loss of scalp and body hair. The disease is unpredictable and may have a significant emotional and psychological impact.
Over the past few years, treatment options have evolved dramatically. This guide explains how alopecia areata is diagnosed, assessed, and managed using current evidence-based strategies.
Understanding Alopecia Areata
What Happens in Alopecia Areata?
In AA, the immune system mistakenly attacks hair follicles, disrupting the normal hair growth cycle. The follicles remain alive, which means regrowth is possible — but relapses are common.
Diagnosis of Alopecia Areata
Clinical Presentation
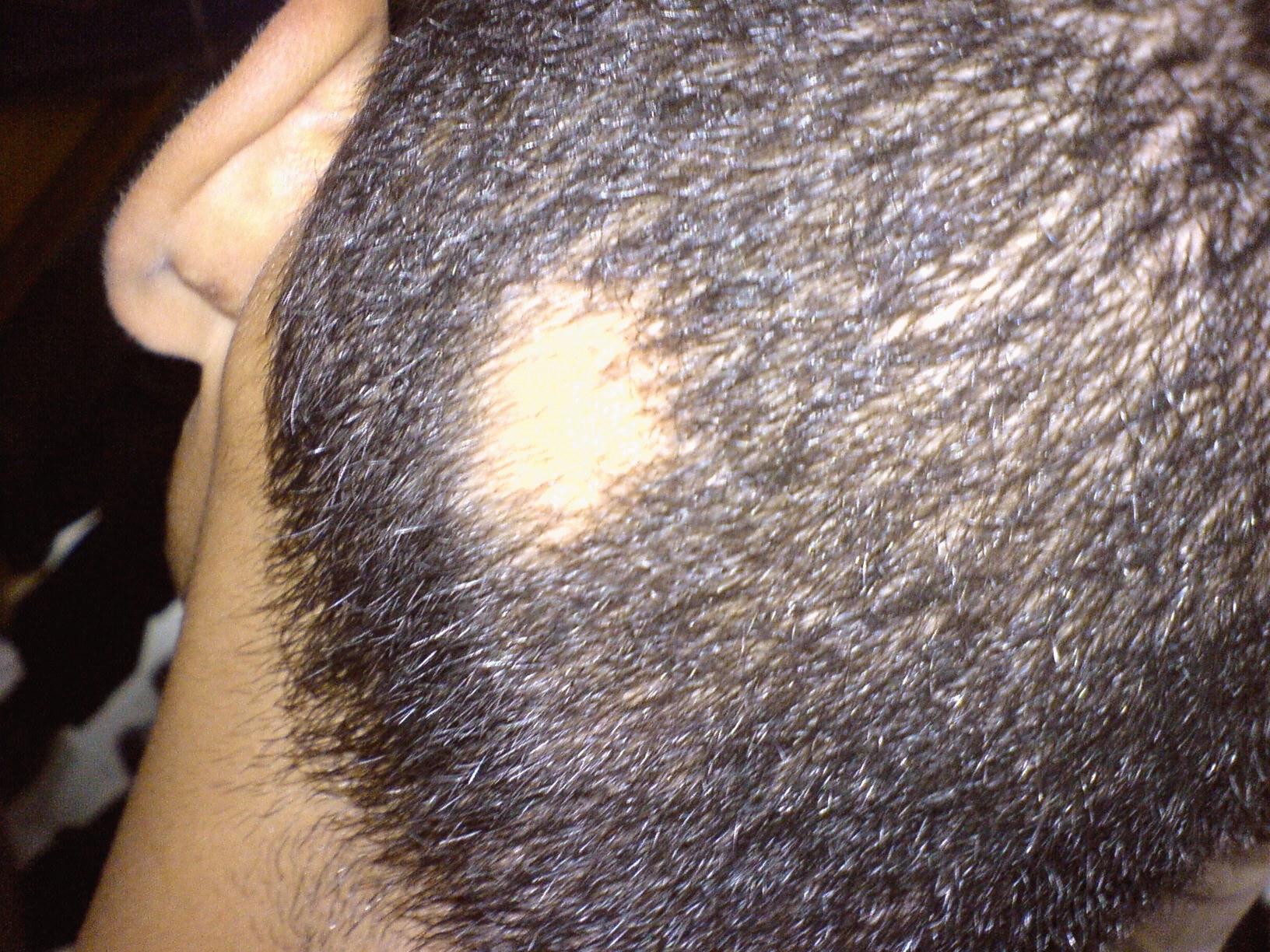
Alopecia areata typically presents as:
Sudden onset of round or oval bald patches
Well-defined, non-scarring areas of hair loss
Smooth underlying skin
A classic sign is “exclamation mark” hairs — short broken hairs that taper near the scalp and are seen at the edge of active patches.
Role of Dermoscopy (Trichoscopy)
Dermoscopy can help confirm diagnosis by identifying:
Black dots (broken hairs at follicle opening)
Yellow dots (follicular keratin plugs)
Broken hairs
Short regrowing vellus hairs

Differential Diagnosis
It is important to rule out other causes of patchy hair loss, such as:
Tinea capitis (fungal infection)
Traction alopecia
Trichotillomania
Telogen effluvium
Associated Conditions
Alopecia areata may be associated with:
Thyroid disorders
Vitiligo
Atopic conditions
Other autoimmune diseases
Nail pitting is commonly seen and may indicate more severe or chronic disease.
Psychological Impact
Hair loss can significantly affect:
Self-esteem
Social confidence
Mental health
Anxiety, depression, and social withdrawal are common. A comprehensive treatment plan must address emotional wellbeing alongside physical management.
Assessing Disease Severity
SALT Score (Severity of Alopecia Tool)
The SALT score measures the percentage of scalp hair loss and helps classify disease severity:
Mild: <20% scalp loss Moderate: 20–49% scalp loss Severe: ≥50% scalp loss This scoring system helps monitor response to treatment. Active vs Stable Disease Active Phase: New patches forming Existing patches enlarging Exclamation mark hairs Possible itching or tingling Stable/Regrowth Phase: No new patches Fine vellus hair regrowth No active symptoms Prognostic Factors Poorer prognosis may be associated with: Early age of onset Nail involvement Extensive scalp involvement (>50%)
Family history of autoimmune disease
Alopecia totalis (complete scalp loss)
Alopecia universalis (total body hair loss)
Relapses are common, especially in patients with previous episodes.
Stepwise Treatment Approach
Management depends on age, severity, progression rate, and psychosocial impact.
Treatment for Mild / Localized Alopecia Areata
(Usually <50% scalp involvement)
Intralesional Corticosteroids
First-line therapy in adults
Triamcinolone acetonide commonly used
Typically injected every 4–6 weeks
Effective for patchy disease
Lower concentrations reduce risk of skin thinning.
Topical Corticosteroids
Preferred for children
Useful for patients unwilling to take injections
High-potency steroids such as clobetasol are commonly prescribed
Adjunct Therapy
Topical minoxidil may enhance regrowth but is not primary therapy.
Treatment for Moderate-to-Severe Alopecia Areata
(≥20% scalp loss or rapid progression)
JAK Inhibitors – A Major Breakthrough
Janus kinase (JAK) inhibitors target immune pathways involved in AA.
They are now considered first-line systemic therapy for moderate-to-severe disease.
Examples include:
Baricitinib
Ritlecitinib
Deuruxolitinib
Clinical trials show significant regrowth in a substantial proportion of patients after 24–36 weeks of treatment.
Important Considerations:
Long-term treatment is often required
Discontinuation may lead to relapse
Careful screening is necessary before starting therapy
Monitoring for infections and cardiovascular risk is essential
Systemic Corticosteroids
Used for:
Rapidly progressive disease
Short-term control
However, relapse rates are high after discontinuation and long-term use is limited by side effects.
Conventional Immunosuppressants
Options include:
Methotrexate
Cyclosporine
Generally considered second-line therapies.
Contact Immunotherapy (DPCP)
Induces allergic reaction to redirect immune response
Used in chronic extensive cases
Requires specialist supervision
Pediatric Management
Children require cautious treatment planning:
High-potency topical corticosteroids preferred
Injections used selectively
Certain systemic treatments approved for adolescents
Management must balance safety with effectiveness.
Emerging Therapies
Research continues in:
Newer JAK inhibitors
Laser-assisted drug delivery
Microneedling combined with topical therapies
The treatment landscape continues to evolve rapidly.
Long-Term Management Strategy
Alopecia areata is often relapsing.
Best practice includes:
Reassessing therapy if no improvement within 24–36 weeks
Continuing treatment 6–12 months after regrowth
Maintenance therapy in severe cases
Ongoing psychological support
Continuous therapy is often required with systemic treatments.
Conclusion
Alopecia areata management has advanced significantly with the introduction of targeted immunotherapies such as JAK inhibitors. However, successful treatment requires more than medication alone.
Effective care depends on:
Accurate diagnosis
Objective severity assessment
Individualized treatment planning
Monitoring for relapse
Addressing psychological impact
With a structured and evidence-based approach, meaningful hair regrowth and improved quality of life are achievable for many patients.
❓ Alopecia Areata – Frequently Asked Questions (FAQs)
1. What is alopecia areata?
Alopecia areata is an autoimmune condition in which the immune system mistakenly attacks hair follicles, leading to sudden, patchy hair loss on the scalp or other parts of the body.
2. What causes alopecia areata?
It is caused by immune system dysfunction. Genetic predisposition, environmental triggers, stress, and viral infections may contribute. It is not caused by poor hair care or nutritional deficiency alone.
3. Is alopecia areata contagious?
No. It is not infectious and cannot spread from person to person.
4. Who is at risk of developing alopecia areata?
It can affect:
Children and adults
Both men and women
Individuals with a family history of autoimmune disorders
People with thyroid disease, vitiligo, or type 1 diabetes
5. What are the symptoms?
Round or oval smooth bald patches
Sudden hair shedding
“Exclamation mark” hairs (short broken hairs at patch edges)
Nail changes such as pitting in some patients
6. Can alopecia areata affect beard or eyebrows?
Yes. It can affect:
Scalp
Beard area
Eyebrows
Eyelashes
Body hair
7. Will the hair grow back?
In many cases, yes. Hair often regrows within months. However, recurrence is common, and some patients may experience repeated episodes.
8. What are the types of alopecia areata?
Patchy alopecia areata (most common)
Alopecia totalis (complete scalp hair loss)
Alopecia universalis (complete body hair loss)
Diffuse alopecia areata (thinning without clear patches)
9. How is alopecia areata diagnosed?
Diagnosis is usually clinical (by examination). In uncertain cases:
Dermoscopy (trichoscopy)
Hair pull test
Rarely, scalp biopsy
10. What treatments are available?
Common treatments include:
Topical or intralesional corticosteroids
Topical minoxidil
Topical immunotherapy
Oral corticosteroids (selected cases)
Baricitinib (JAK inhibitor for severe cases)
Other JAK inhibitors in resistant cases
Treatment choice depends on age, severity, and duration.
11. Is alopecia areata permanent?
Not always. Many patients experience spontaneous regrowth. However, severe forms (totalis or universalis) may be persistent.
12. Does stress cause alopecia areata?
Stress does not directly cause it but may trigger or worsen an episode in susceptible individuals.
13. Can diet cure alopecia areata?
There is no proven dietary cure. However, correcting vitamin D deficiency, iron deficiency, or other nutritional imbalances may support hair health.
14. Is hair transplantation useful?
Hair transplant is generally not recommended because the autoimmune process can attack transplanted follicles.
15. When should I see a doctor?
Consult a dermatologist if:
Sudden patchy hair loss occurs
Hair loss spreads rapidly
Eyebrows or eyelashes are affected
There is associated nail change
